
Shadow Health has a wide range of simulation characters, or Digital Standardized Patients™, that allow students to practice clinical skills in nursing disciplines from Fundamentals to Advanced Primary Care. Because of the patented natural language Conversation Engine within Shadow Health’s Digital Clinical Experiences™ (DCEs), students can practice authentic conversations with patients with diverse representation that students may not see in the clinical setting.
Shadow Health understands the importance of allowing students the opportunity to interact with patients in a respectful, meaningful, and accurate way. It takes a large team of collaborators to create screen-based simulation offerings—including a cross-functional team of Nurse Educators, Developers, Artists, Technical Sound Designers, Learning Designers, Narrative Designers, Product Managers, and Scrum Managers. They make it their priority to incorporate optimal learning opportunities with realistic conversation and empathy to each of the simulated patients to truly make them virtual human beings who breathe, blink, and have rich and complex histories.
Here are some examples of patients in Shadow Health representing diverse backgrounds and ensuring students can practice therapeutic communication.
Anita Douglas

Anita Douglas is a 72-year-old Black woman who appears in both graduate and undergraduate DCEs. Anita appears in Advanced Pharmacology and Advanced Diagnostics DCEs for graduate students. In the Advanced Diagnostics DCE, Anita has been experiencing fatigue and weakness that has impaired her activities of daily living for a few months and has had her symptoms dismissed as ‘old age’.
Daanis LaFontaine

Daanis LaFontaine, 18, is a member of the Turtle Mountain Band of Chippewa Indians, an Ojibwe people. Assignments featuring Daanis and our other Native American characters were developed in partnership with Dr. Misty Wilkie, an enrolled member of the Turtle Mountain Band of Chippewa Indians and a nurse who grew up on the Turtle Mountain Indian Reservation in Belcourt, North Dakota.
Daanis LaFontaine and her mother, Rebecca LaFontaine
Fatima Khan

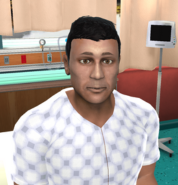
In a Medical-Surgical DCE, students meet Fatima Khan, a 44-year-old type 1 diabetic who is pre-operative and awaiting a laparoscopic cholecystectomy. As part of this simulation, students practice healthcare considerations that may be important to Muslim patients, including diet, modesty and privacy, touch restriction and consent, and substance use restriction.
Felipe Barbosa
Felipe Barbosa is a 48-year-old Brazilian American man who presents with a rash in a primary care setting in the Advanced Primary Care – Adult Management DCE. Felipe is in a healthy, happy marriage and has been married to his husband, Marvin, for three years. He is proud of his work as a firefighter, but a recent traumatic episode caused resulting grief.
Lupe Sosa

Lupe Sosa, 21, is a college student who balances a full academic schedule as a philosophy and music double major, along with a work/study job at the library, DJ gigs in local nightclubs, club fencing, and vibrant relationships with their friends and family. Lupe is gender non-binary and uses they/them pronouns. Non-binary people do not identify with the binary gender identities of man or woman. Students can meet Lupe in the Advanced Primary Care: Mental Health* DCE. In the scenario, students help Lupe consider the possible cause of their sleep disturbances.
Quan Van Tran

When students first meet Quan Van Tran, 50, they encounter him in a clinical setting shortly after he has received a positive diagnosis of HIV. Quan is a Vietnamese American who immigrated to the United States. In previous years, research shows the number of HIV diagnoses among Asians in the U.S. increased, and 1 in 5 Asians living with HIV in the U.S. did not know they had it. Quan also does not think of himself in terms of sexual orientation.
Tanner Bailey

Tanner Bailey is a 30-year-old transgender man who works as a theatre director at a queer theatre company. In his spare time, he loves working out and watching old movies. He is proactive about his health and happiness. Tanner appears in two different simulations in Advanced Pharmacology and Community Health DCEs, where cases highlight the difficulties trans people face on a daily basis due to unjust bias including regular discrimination in health care and the job sector.
Xavier Daniels

Xavier Daniels is a 54-year-old Black man who has come to the clinical for an establishing care visit during the Advanced Primary Care: Adult DCE. He was laid off three years ago and did not have health insurance until beginning his current job as an electrician two months prior to this visit. Xavier last saw a provider three and a half years ago, at which point he was diagnosed with high blood pressure. He felt dismissed by this provider, who did not offer education about high blood pressure management and insinuated Xavier would not be able to afford future visits.
Zachary LaFontaine

In the Advanced Primary Care – Pediatrics DCE, students have the opportunity to interact with Daanis and her son Zachary. Students care for Zachary as an infant at his 2-month well visit and then in a later assignment when Zachary is a toddler for a sick visit.
Zachary LaFontaine with Daanis’s mom, Rebecca
What this means for nursing students
Research indicates that change is necessary for healthcare to eliminate bias, reduce health disparities, and consider the impact of social determinants of health for patient care (Carter, 2020). While preceptors can guide students on social context or special considerations to keep in mind during a patient interaction in the clinical setting, students can practice interacting with virtual human beings from different backgrounds and engage in thoughtful, empathetic communication through means like screen-based virtual simulations. This not only streamlines student learning but guarantees they have the opportunity to practice respectful interactions with a diverse range of patients.
Contributions and revisions of this piece were done in part with Watson Nelson Consulting, a partner with Shadow Health to ensure matters of diversity, equity, and inclusion are accurately represented with simulation characters. Learn more about Watson Nelson Consulting.
Resources
Altmiller, G., Jimenez, F., Wharton, J., Wilson, C. (2022). HIV and Contact Tracing: Impact of a Virtual Patient Simulation Activity. Clinical Simulation in Nursing, 64. 58-66. https://doi.org/10.1016/j.ecns.2021.12.005
Carter, B. (2020). Achieving diversity, inclusion and equity in the nursing workforce. Revista latino-americana de enfermagem, 28, e3254. https://doi.org/10.1590/1518-8345.0000-3254
CDC. (2022, April 14). HIV in the United States by Race/ethnicity. Centers for Disease Control and Prevention. Retrieved May 5, 2022, from https://www.cdc.gov/hiv/group/racialethnic/other-races/index.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fhiv%2Fgroup%2Fracialethnic%2Fasians%2Findex.html
Felias-Christensen, G, Corl, D. (2010, January 1). Muslim Religious Observances and Diabetes. Retrieved from https://ethnomed.org/resource/muslim-religious-observances-and-diabetes/
Kcomt, L., Gorey, K. M., Barrett, B. J., & McCabe, S. E. (2020). Healthcare avoidance due to anticipated discrimination among transgender people: A call to create trans-affirmative environments. SSM – Population Health, 11, 100608. https://doi.org/10.1016/j.ssmph.2020.100608
Kroning, M. (2018) Lesbian, Gay, Bisexual, and Transgender Education in Nursing. Nurse Educator, 43(1), 41. doi: 10.1097/NNE.0000000000000429
Lynn, V., Watson, C., Giwa-Onaiwu, M., Ray, V., Gallagher, B., & Wojciechowicz, V. (n.d.). HIV #LanguageMatters: Addressing Stigma by Using Preferred Language. HIVE. Retrieved March 10, 2022, from https://hiveonline.org/wp-content/uploads/2016/01/Anti-StigmaSign-Onletter-1.pdf
National LGBT Health Education Center. (n.d.). Providing affirmative care for patients with non-binary gender identities. lgbthealtheducation.org. Retrieved September 7, 2022, from https://www.lgbtqiahealtheducation.org/wp-content/uploads/2017/02/Providing-Affirmative-Care-for-People-with-Non-Binary-Gender-Identities.pdf
Patterson, J. G., Tree, J. M. J., Kamen C. (2019). Cultural competency and microaggressions in the provision of care to LGBT patients in rural and appalachian Tennessee. Patient Education and Counseling, 102 (11). 2090. https://doi.org/10.1016/j.pec.2019.06.003
Pew Research Center. (2011, August 30). Muslim americans: no signs of growth in alienation or support for extremism. Section 1: a demographic portrait for muslim americans. Retrieved from: https://www.pewresearch.org/politics/2011/08/30/section-1-a-demographic-portrait-of-muslim-americans/
Pew Research Center. (2018, April 17). Muslims in America: Immigrants and those born in U.S. see life differently in many ways. Retrieved from: https://www.pewforum.org/essay/muslims-in-america-immigrants-and-those-born-in-u-s-see-life-differently-in-many-ways/
Sherman, A. D., McDowell, A., Clark, K.D., Balthazar, M., Klepper, M., Bower, K. (2021) Transgender and gender diverse health education for future nurses: Students’ knowledge and attitudes. Nurse Education